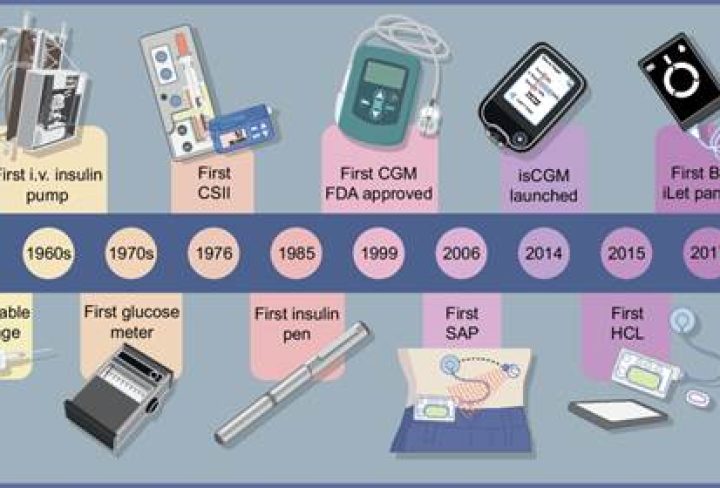
In the realm of diabetes management, the introduction of Continuous Glucose Monitoring (CGM) technology has marked a revolutionary shift. CGMs are redefining how people with diabetes monitor their health, providing real-time data that helps make informed decisions.
An Introduction to Continuous Glucose Monitoring (CGM)
For years, managing diabetes meant relentless daily routines — from meal planning to frequent finger-pricks. Imagine Jane, who has to prick her finger multiple times a day to check blood sugar levels. Missing even a couple of readings could lead to unexpected highs or lows, posing significant health risks. Here lies the transformative power of CGM technology.
CGM offers a new way forward, marking a departure from traditional, often cumbersome methods. Unlike traditional methods requiring multiple daily finger-pricks, a CGM device provides continuous readings throughout the day and night. This means less discomfort and a more comprehensive picture of what’s happening inside the body.
There are myths afloat about CGMs being complicated or unreliable. However, ease of use and reliability set CGMs apart from any other tools. CGMs consist of a small sensor, typically attached to the skin, which automatically records glucose levels. This shift not only translates to convenience but also enables better diabetes management. With a bit of learning, gone are the days of tedious monitoring routines, making these devices a game-changer for many.
How Does CGM Technology Work?
Understanding how does CGM work reveals its simplicity. A CGM system has three main parts:
- Sensor: This is inserted just under the skin, often on the abdomen or arm. The sensor measures glucose in the interstitial fluid.
- Transmitter: Attached to the sensor, it sends data wirelessly.
- Receiver or Smart Device: This is where you view your glucose levels, trends, and alerts.
So, how does a CGM device work in practical terms? It starts with inserting a tiny sensor, which is barely felt once in place. This flexibility means more freedom for users, allowing them to carry on their usual activities with minimal disruption.
Once the sensor detects glucose levels, the transmitter sends this information to a receiver or even directly to a smartphone app. Users get continuous updates, and with how does CGM work efficiently, they’re alerted if levels fall outside a safe range, either too high or too low. This real-time data is invaluable, allowing immediate action.
These sensors can be worn round-the-clock for several days. Depending on the model, a user might replace a sensor every week or two. This longevity ensures less interference with daily life while providing consistent monitoring. It’s important to choose the right location on the body for the sensor for optimal performance, often based on comfort and ease of access.
The Advantages and Impact of CGM on Diabetes Management
What advantages does the CGM device work offer? Here’s a snapshot:
- Continuous Monitoring: Unlike a single reading from a finger prick, CGMs provide a constant stream of data, making it possible to see trends over time.
- Improved Management: With continuous tracking, there are fewer emergencies or surprises. Users can predict potential problems before they happen, promoting better decision-making.
- User Empowerment: Having access to ongoing data means users can make lifestyle changes confidently, knowing they have accurate, timely information.
Integration with smartphones makes it even easier. Users not only track their data but also share comprehensive reports with healthcare providers. This integration fosters a team-based approach to care and ensures all stakeholders are informed and involved. Real-life stories abound, with users experiencing newfound freedom and peace of mind. Many report feeling empowered to lead more normal, unrestricted lives, fundamentally changing their day-to-day outlook.
Navigating the Future and Addressing Concerns
Looking to the future, CGM technology promises even more. Anticipated advancements might include further integration with insulin pumps and the evolution into closed-loop systems, which could operate almost like an artificial pancreas. These emerging technologies will simplify management further, offering seamless control with less manual intervention.
However, financial considerations cannot be overlooked. CGMs can be costly, and access depends largely on healthcare coverage. Addressing economic barriers is essential to ensure broader accessibility. Users should explore their insurance policies or talk with healthcare providers to understand their options better.
Privacy is another aspect of interest. Today’s CGM devices work with robust security measures to protect user information. Understanding and trusting these systems is key for users concerned about data security. As technology advances, these systems are continually updated to address any vulnerabilities.
In conclusion, CGMs represent a significant leap forward in diabetes care. Those curious about how CGM works are encouraged to have conversations with their healthcare providers. With ever-improving technology, the horizon is bright, offering hope and improved health for those living with diabetes.